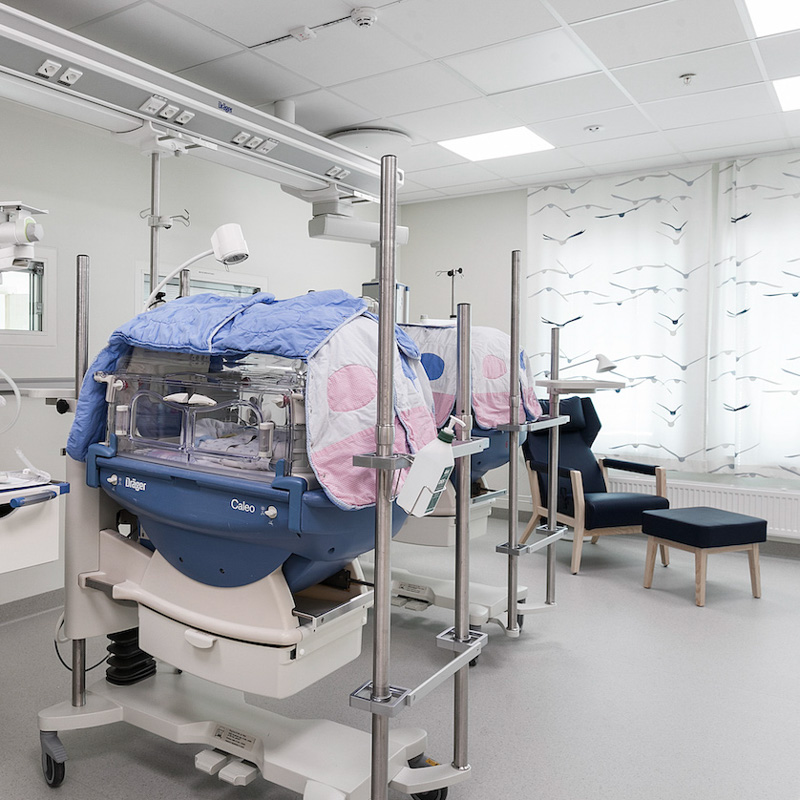
Healthcare
Daylight promotes health.
Daytime exposure to high illuminances, from either sunlight or a few hours of bright-light therapy, is known to have beneficial effects on clinical parameters such as recovery, length of stay, depression and agitation.
But in many healthcare facilities access to daylight is limited. Individual human needs put high requirements on indoor lighting in these environments. Biocentric lighting is designed to deliver the right amount of circadian stimulus at the right time of day, helping patients recover faster and staff perform better.
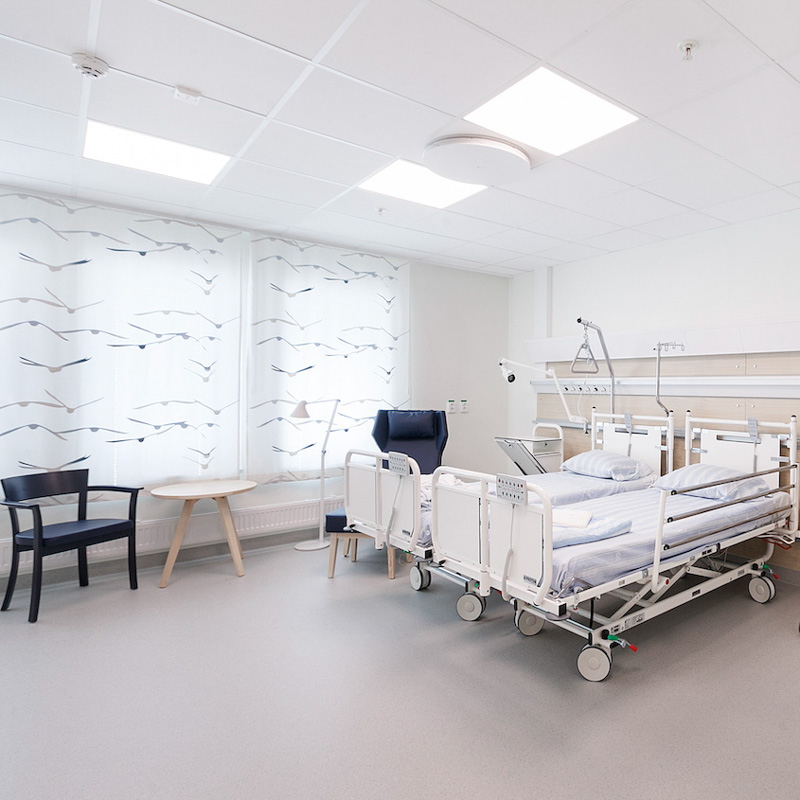

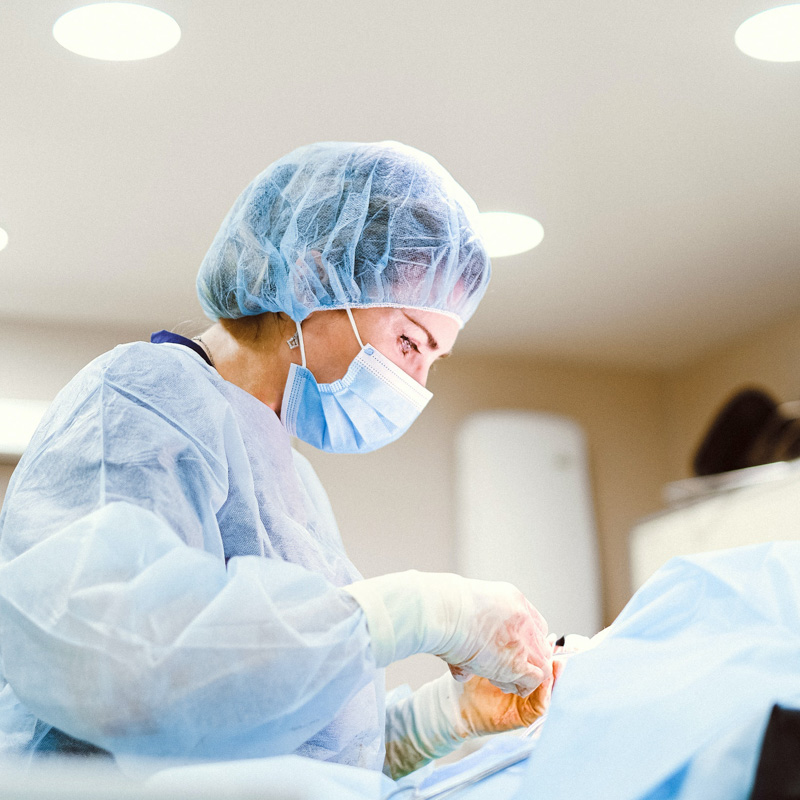
Setting new standards for healthcare.
Current standards and guidelines for lighting systems within patient rooms typically specifies horizontal illuminance thresholds as low as 100 lux¹, a level insufficient to generate the same benefits as natural daylight (2000–100 000 lux) under which we have evolved. Not surprisingly, hospitalized patients often suffer from sleep and circadian rhythm disruption².
With Biocentric lighting, we deliver a higher circadian stimulus than industry norms of similar lighting solutions, which further promotes health benefits associated with the light environment.

Benefits of Biocentric lighting
- Improve shift work
- Promote patient recovery
- Better sleep
Examples of application areas
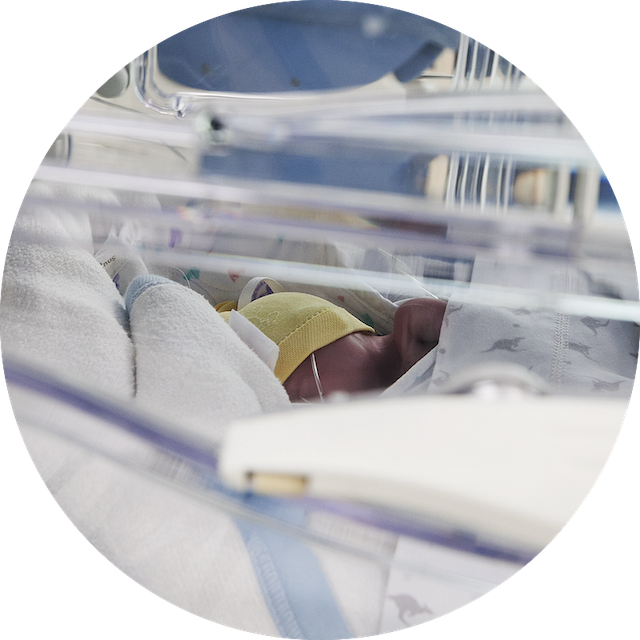
Neonatal
Keeping prematurely born children in a continuously dark or continuously lit environment while in the NICU, deprives them of the circadian stimuli they would have received during pregnancy. At Helsingborg Hospital, the light environment is adapted to meet the biological needs of both babies, parents and the staff.

Elderly care
Elderly have different needs compared to younger individuals. In care facilities, it is usual for elderly to spend the majority of time indoors, which may prevent them from sustaining their circadian rhythm.
Acute care
Acute care patients typically dwell in low levels of light, which may limit their exposure to the light they need. Not surprisingly, circadian dysrhythmias are often found, and hospitalized patients often suffer from sleep and circadian rhythm disruption.
Shorten length of stay
With higher levels of light intensity, length of stay can be reduced. A study from 2013 found that length of stay was reduced by 7.3 hours per 100x increase of daylight inside.³
Improve shift work
Many shift workers experience sleepiness at work which can increase the risk of human error. Use of adapted light can therefore be appropriate to help reduce fatigue. ⁴
Minimize risks with disinfection
Secure sanitary spaces for staff and patients. BrainLit UVen uses UV-C lighting to quickly, safely and automatically disinfect both air and surfaces to create a safe and healthy environment.
Higher accuraccy in examinations
Cinical examination of preterm babies and their skin demands a good perception of color. Biocentric lighting provides a CRI that is above the industry requirement.
Shorten length of stay
With higher levels of light intensity, length of stay can be reduced. A study from 2013 found that length of stay was reduced by 7.3 hours per 100x increase of daylight inside.³
Improve shift work
Many shift workers experience sleepiness at work which can increase the risk of human error. Use of adapted light can therefore be appropriate to help reduce fatigue. ⁴
Minimize risks with disinfection
Secure sanitary spaces for staff and patients. BrainLit UVen uses UV-C lighting to quickly, safely and automatically disinfect both air and surfaces to create a safe and healthy environment.
Higher accuraccy in examinations
Cinical examination of preterm babies and their skin demands a good perception of color. Biocentric lighting provides a CRI that is above the industry requirement.
Experience the difference.
Downloadable Materials
References
- Svensk standard SS-EN 12464-1:2021. Ljus och belysning – Belysning av arbetsplatser – Del 1: Arbetsplatser inomhus.
2. Tan X, van Egmond L, Partinen M, Lange T, Benedict C. A narrative review of interventions for improving sleep and reducing circadian disruption in medical inpatients. Sleep Med. 2019;59:42-50. doi:10.1016/j.sleep.2018.08.007
3. Joarder AR, Price A. Impact of daylight illumination on reducing patient length of stay in hospital after coronary artery bypass graft surgery. Light Res Technol. 2013;45(4):435-449. doi:10.1177/1477153512455940
4. J.A. Olson, D. Z. Artenie, M. Cyr, A. Raz, V. Lee, Developing a light-based intervention to reduce fatigue and improve sleep in rapidly rotating shift workers. Chronobiol Int37, 573-591 (2020).